Flashback Friday - Insulin and the 'Wandering Diabetic Nurse'
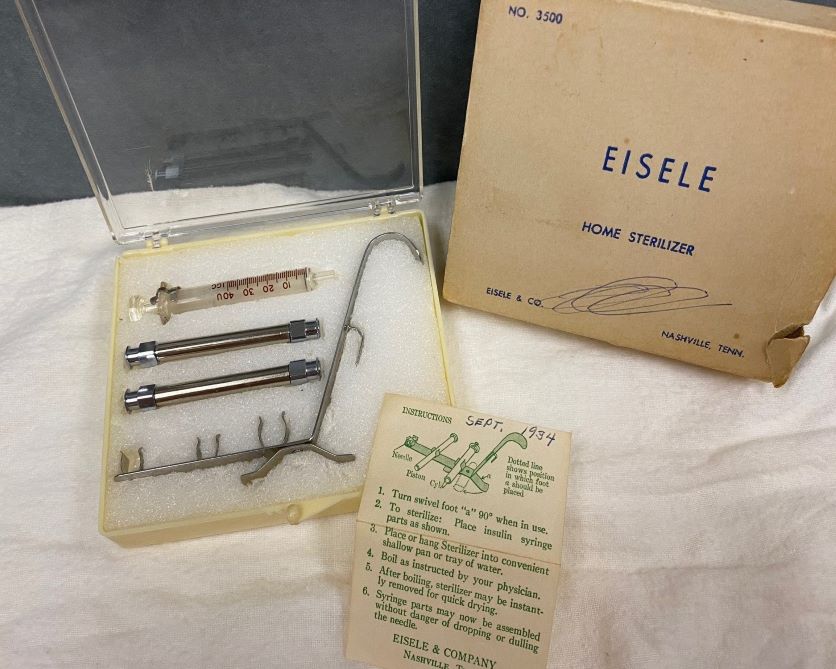
A peculiar artifact in the Bjoring Center’s archives prompted us to post a challenge on social media recently for anyone to identify it. No one could. Creative but incorrect answers ranged from a paper holder to an x-ray film hanger.
Our mystery object is part of a home sterilizer kit for insulin syringes, manufactured in the early 1930s by Eisele & Co. of Nashville, Tenn. The original instruction sheet, hardly bigger than a matchbook, is also preserved.
The kit is pocket-sized and simple, but managing diabetes during this era was anything but. When insulin was discovered in the 1920s, the nursing care for a diabetic was intensive, complicated and—it goes without saying—monumentally time-consuming. Tasks included collecting the patient’s urine to measure levels of glucose and albumin; weighing carbohydrates, fats, and proteins as part of strict dietary regimens; multiple daily injections of insulin; and the near-constant cleaning, sharpening, and sterilizing of the equipment. Diabetic patients also needed exercise and diversions to help them cope with this disease.
"It is within my memory that diabetes was quickly fatal in children and spoken of as a dreaded disease,” nurse Marjorie A. Everingham wrote in the American Journal of Nursing in 1932. “Today, the diabetic child, while limited in certain respects, has equal opportunities with other children for an interesting and useful life.”
Insulin was life-changing, but access to skilled nursing care was decidedly unequal. Only the wealthy could afford to hire a private duty “diabetic nurse” for a stricken family member—for weeks, months, sometimes many years. It was beyond the reach even for middle-class families.




Many of the nurses who wanted to specialize in diabetes care were trained by Boston physician Elliott P. Joslin at New England Deaconess Hospital. Joslin believed that nursing care outside of the hospital was better for the families. Working in the home, these trained nurses “are often of more value to the patient than is the doctor,” he said.
In 1928, a graduate of New England Deaconess Hospital named Lovilla E. Winterbottom became the first “Wandering Diabetic Nurse.” In this role, a nurse could “wander in whatever direction diabetic patients might call her,” Winterbottom explained in the American Journal of Nursing. They visited patients regardless of their financial status or race and were “met with the upmost appreciation and cooperation,” she added. A philanthropic fund paid their salaries but this novel program was limited to Massachusetts and New York City.
The Wandering Diabetic Nurse would remain in a household for as long as she felt was necessary; empowering patients to care for themselves was key. Family members also needed instruction in computing food values, preparing meals, treating insulin reactions, and myriad other round-the-clock decisions.
“Recently, one of our nurses in the course of two months visited 20 private homes and gave 460 interviews to patients in the hospital in addition to some classroom instruction,” Joslin wrote in 1931, in Diabetes: Its Control by the Individual and the State. He added, “A day spent by a nurse in teaching in a diabetic child’s home is worth a week of care of that same child in a hospital.”
By 1941, however, Joslin reported at a New York Academy of Medicine meeting that “we have given up our Wandering Diabetic Nurse, going from home to home, because we no longer needed her.” What spelled her obsolescence? Technological advances—in this case, the introduction of protamine zinc insulin, which made treatment easier and kept diabetes under better control.
###
Today’s #FlashbackFriday is brought to you by the Bjoring Center for Nursing Historical Inquiry at UVA, which is dedicated to the preservation and study of nursing history.

