Community Exposures: A Day in the Life of Community Health Nursing Clinical Rotations
 It’s a Thursday morning, and between the near-constant stream of children with coughs, upset stomachs and headaches, fourth-year University of Virginia nursing student Mary Shields ticks off what makes for a typical day in Moss Nuckols Elementary School nurses’ office, where she spends each Thursday.
It’s a Thursday morning, and between the near-constant stream of children with coughs, upset stomachs and headaches, fourth-year University of Virginia nursing student Mary Shields ticks off what makes for a typical day in Moss Nuckols Elementary School nurses’ office, where she spends each Thursday.
Temperature-taking for the possibly feverish. Pupil exams for head bumps. Paper towel pressure to compel nosebleeds into submission. And handwashing, handwashing, handwashing.
Then there are the more serious tasks: medications – Ritalin, insulin injections, digestive enzymes – which are dispensed by the school’s registered nurse, Tabitha Smith. Lice (“Live lice, they go home, but just eggs, they can stay,” Shields notes). Blood sugar checks and care for chronic conditions, like diabetes and hemophilia – issues that Shields hadn’t seen up close, despite having had a clinical rotation in a hospital pediatrics unit.
Shields’ semester-long community health course – which requires 84 hours of clinical work, including her weekly gig at Moss Nuckols – has been a lesson in the expansive role of a community health nurse. And school nurse isn’t the only role she’s played.
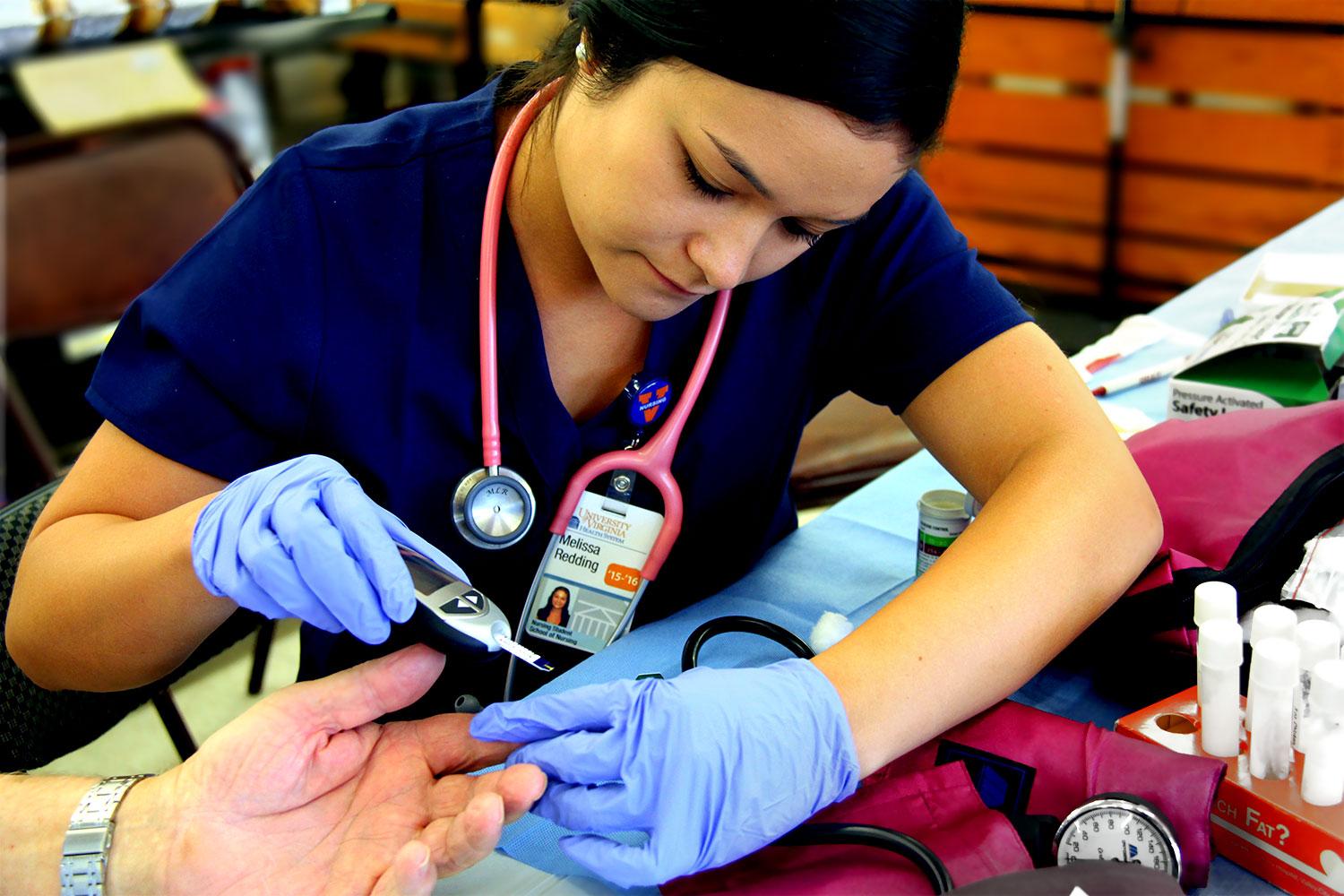
She, along with seven of her peers, also made presentations about health warning signs to pews full of parishioners at a national Pentecostal conference. They’ve pricked shoppers’ fingers (to measure blood sugar) and cuffed their arms (to check blood pressure) amid fresh produce and donuts during a health screening at the local grocery store. They’ve taught middle- and high-schoolers CPR and the Heimlich maneuver, described the rewards of nursing to high-schoolers enrolled in certified nursing assistant courses, even had their ears nudged with acupuncture needles for a unit on complementary and alternative therapies – all under the watchful eye of clinical instructors like Vickie Southall, a veteran community health nurse and UVA Nursing clinical instructor who grew up and resides in Louisa and remains a beloved and well-connected pillar of that community today.
That’s been true for Shields, who’s discovered that nurses provide a critical, holistic set of eyes: Are there kids with repeat, unresolved cases of lice? Children who need asthma medications their parents can’t afford? Students who arrive at school dirty, hungry or poorly shod? With tell-tale bruises or unexplainable injuries? With cavities, and no way to get dental care?
“It’s a huge scope that I wasn’t really aware of,” said Shields, noting that the school nurse is sometimes the first point of contact in cases of suspected abuse or neglect.
It’s a sentiment echoed by fourth-year students Liza Wayland and Kate Rossbach, who spend each Thursday at Louisa’s food bank taking care of what needs to be done: checking blood pressures, answering residents’ medication questions, even researching recipes for the pantry’s more obscure donated vegetables, like yucca, guava and “zoodles” (shaved zucchini that can be used in the place of pasta). With food pantry staffers, the duo also helps assemble large pallets of food for clients who arrive every few minutes to take their monthly allotment of food, sometimes wrestling the donations across the parking lot and into car trunks or truck flatbeds.
“We talk a lot about how, at UVA, we live in a bubble,” Rossbach said. “But coming to a rural area where generational poverty is common – the mom will be driving, and there’s the grandma in the passenger seat, and an 8-year-old in the back – it’s amazing to see the resources that are in place in a town this small. And the food bank is a completely safe, non-judgmental space.”
For fourth-year student Heather Kesler, who helps care for patients at Louisa County’s only prenatal clinic – run out of a small, tidy trailer that lies snug against a Louisa pine forest – patient diversity has proven the biggest eye-opener.
Kesler – who, having grown up on a Franklin County dairy farm, is no stranger to rural poverty – regularly helps navigate patients’ worries about transportation, and listens to their financial fears and relationship instabilities. And while it’s also a chance for her to practice drawing blood, administering fetal stress tests and screening for sexually transmitted diseases, perhaps her most constant role is to assuage the anxiety many of her patients feel before giving birth – or after.
“They ask, ‘Will I be a good mother? Can I do this? Do I want to do this?’” Kesler said. The lessons she’s learned are palpable, and she notes her satisfaction in developing trust with her patients, especially through repeat exposures.
“[My work here] is going to stick with me,” she said.
That’s edifying to Southall and Camille Burnett, a School of Nursing professor and the academic director of its community engagement and partnerships programs.
“Public health nursing is rooted in exploring and shaping community health by ensuring conditions facilitate optimal health and wellbeing,” Burnett said, “and it’s our job to expose students to the broad spectrum of the profession and those things that determine health outcomes for the communities and families within.”
“Connecting with the community and developing insight about the difficult health choices families face are the course’s two big takeaways,” Southall added. “That, and learning that health care begins in the community – and nurses often make all the difference.”
###





